Understanding Oral Granulomatous Disease in Everyday Terms
Oral granulomatous disease is a medical condition that affects the mouth and surrounding tissues, creating chronic inflammation known as granulomas. These granulomas are clusters of immune cells that form in response to long-term irritation, infection, or other underlying health issues. In the U.S., dental professionals often encounter patients with unexplained swelling, ulcers, or lumps in the oral cavity, and further evaluation may reveal granulomatous inflammation. The condition is complex because it can be linked to systemic diseases like Crohn’s disease, sarcoidosis, or even allergic reactions. For patients, the symptoms may start subtly, such as mild gum swelling or persistent sores, before progressing into visible and sometimes painful oral changes. Recognizing what oral granulomatous disease looks like is key to getting early treatment and preventing complications.
1. Symptoms That Signal Oral Granulomatous Disease
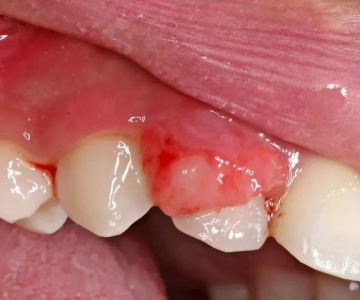
The symptoms of oral granulomatous disease vary, but they typically involve persistent swelling or inflammation in the mouth. Patients often notice thickened lips, swelling inside the cheeks, or lumps that don’t heal on their own. In some cases, painful ulcers or fissures on the gums and tongue develop. Difficulty eating, speaking, or swallowing may occur when inflammation becomes severe. A real-life example involves a patient who initially thought she had a minor mouth infection but experienced worsening swelling over weeks. After evaluation, her dentist discovered granulomatous changes linked to Crohn’s disease. This story highlights how oral symptoms can sometimes be the first clue to an underlying systemic problem. For U.S. patients, especially those with chronic conditions, monitoring these early warning signs is vital.
2. Causes Behind Granulomatous Inflammation in the Mouth
Understanding the causes of oral granulomatous disease requires looking at both local and systemic triggers. Locally, dental infections, poorly fitted prosthetics, or foreign bodies like dental materials may provoke granuloma formation. Systemically, diseases such as Crohn’s disease, tuberculosis, and sarcoidosis often present with oral manifestations. Allergic reactions to food additives, cinnamon, or benzoates can also spark inflammation. Research shows that in some cases, no clear cause is found, leaving the condition classified as idiopathic. For patients, the uncertainty can be frustrating, but identifying triggers with the help of a dentist or specialist is the first step in treatment. This connection between oral health and whole-body health underscores the importance of comprehensive medical and dental evaluations in the United States.
3. How Oral Granulomatous Disease Is Diagnosed
Diagnosis of oral granulomatous disease is not straightforward, as it requires ruling out multiple possible causes. Dentists often begin with a detailed medical history and physical examination. If granulomatous lesions are suspected, a biopsy is usually performed to analyze the tissue under a microscope. This helps distinguish granulomatous disease from oral cancers, fungal infections, or other inflammatory conditions. Blood tests and imaging studies may be ordered to check for systemic diseases like Crohn’s or sarcoidosis. A case study from a dental clinic in New York revealed that a patient with persistent gum swelling had granulomatous inflammation caused by an allergic reaction to a food preservative, something only discovered after detailed testing. This process shows why professional diagnosis is essential and why patients should not ignore persistent oral swelling.
4. Treatment Options for Managing Oral Granulomatous Disease
Treatment depends on the underlying cause of the disease. If it is related to a systemic condition like Crohn’s, managing the primary disease often improves oral symptoms. Corticosteroids, either topical or systemic, are commonly prescribed to reduce inflammation. In cases caused by allergies, eliminating the triggering substance can lead to significant improvement. Surgical intervention may be necessary if granulomas are large or interfere with oral function. For many patients, a combination of medical and dental care is needed to achieve lasting results. One patient story highlights this: a man with sarcoidosis experienced severe lip swelling that made speaking difficult. After treatment with systemic steroids and ongoing dental monitoring, his condition improved, allowing him to return to normal daily activities. This demonstrates how timely treatment can restore both health and quality of life.
5. The Impact on Oral and Overall Health
Oral granulomatous disease affects more than just the mouth. The chronic inflammation can disrupt eating, nutrition, and social confidence. In children and young adults, the condition may lead to missed school or workdays due to pain and discomfort. Moreover, the disease can indicate hidden systemic conditions that require medical attention. For example, patients who present with unexplained oral granulomas may later be diagnosed with Crohn’s disease, an inflammatory bowel condition. This connection between oral and systemic health reinforces the need for a holistic approach to care. Dental clinics across the U.S. often collaborate with medical doctors to ensure comprehensive treatment. Patients who suspect they have oral granulomatous disease should consider professional evaluation not just for oral comfort but for broader health monitoring as well.
6. Living With Oral Granulomatous Disease: Patient Perspectives
Living with oral granulomatous disease can be emotionally and physically challenging. Some patients report feeling embarrassed by visible swelling, while others struggle with eating spicy or acidic foods that trigger discomfort. Support groups and online communities provide encouragement, but professional dental care remains the cornerstone of managing the disease. U.S. patients often share their journeys of trial and error—adjusting diets, undergoing treatments, and finding routines that minimize flare-ups. These personal stories bring awareness to a condition that remains underrecognized. They also highlight the importance of dental education and awareness campaigns to help more patients get early diagnoses. For those seeking professional advice and tailored care, websites like Family Dentistry Online provide resources to connect patients with the right specialists and treatment options.
Conclusion: Why Early Detection and Treatment Matter
Oral granulomatous disease is a complex condition that requires both awareness and action. From subtle swelling to significant granuloma formation, the disease presents in many ways but always signals the need for professional care. The answer to “what is oral granulomatous disease” lies in understanding it as both a dental and medical issue. By recognizing symptoms, identifying causes, and pursuing targeted treatment, patients can manage the condition effectively and avoid long-term complications. Early detection not only improves oral health but may also uncover systemic diseases requiring immediate attention. For U.S. patients, staying proactive and working with dental professionals is the key to protecting both their smile and overall health. If you suspect symptoms of oral granulomatous disease, seeking timely help can make all the difference in recovery and quality of life.



 Hillcrest Dental Group, P.A.4.0 (826 review)
Hillcrest Dental Group, P.A.4.0 (826 review) Salem Orthodontics4.0 (188 review)
Salem Orthodontics4.0 (188 review) Pleasant Smiles Dental4.0 (8 review)
Pleasant Smiles Dental4.0 (8 review) Lake Area Dental4.0 (24 review)
Lake Area Dental4.0 (24 review) Franco Picofazzi DDS, FADSA, PC4.0 (66 review)
Franco Picofazzi DDS, FADSA, PC4.0 (66 review) Robison Dental Group4.0 (197 review)
Robison Dental Group4.0 (197 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile