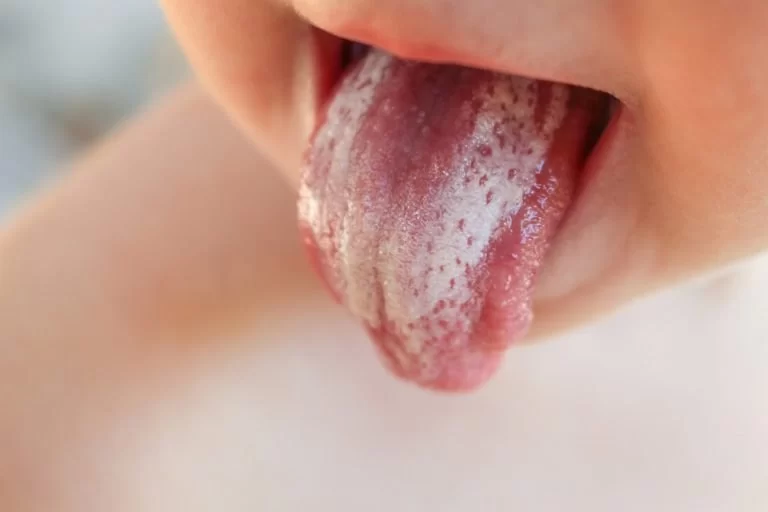
What Autoimmune Diseases Cause Oral Thrush
Oral thrush, also known as oral candidiasis, is a fungal infection caused by the overgrowth of Candida yeast inside the mouth. While anyone can develop this condition, people with weakened immune systems are at higher risk. This includes individuals living with autoimmune diseases, where the body mistakenly attacks its own tissues and disrupts the balance of the immune response. For many patients in the United States, oral thrush is not just a minor annoyance but a recurring problem that signals deeper health concerns. Understanding the connection between autoimmune disorders and oral thrush helps both patients and caregivers manage symptoms more effectively.
Why Autoimmune Diseases Increase the Risk of Oral Thrush
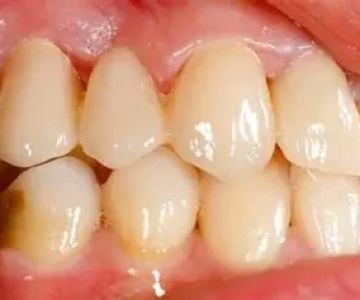
The immune system normally plays a critical role in keeping Candida levels under control. When autoimmune diseases interfere with immune regulation, the body’s defenses may weaken, creating opportunities for fungal infections. Certain autoimmune conditions can also cause chronic dryness in the mouth or require long-term use of immunosuppressive medications, both of which increase the likelihood of oral thrush. Patients often describe feeling a burning sensation on the tongue, white patches inside the cheeks, or difficulty swallowing—common signs that yeast overgrowth is occurring.
Autoimmune Diseases Most Commonly Associated with Oral Thrush
Several autoimmune conditions are directly linked to higher rates of oral thrush:
- Sjögren’s Syndrome: This autoimmune disorder targets the glands that produce saliva and tears. Reduced saliva flow creates a dry environment where Candida thrives, making oral thrush a frequent complication.
- Lupus (Systemic Lupus Erythematosus): Lupus patients often undergo immunosuppressive treatments, lowering their body’s ability to fight infections like oral thrush. The disease itself can also affect the mucous membranes in the mouth.
- Rheumatoid Arthritis: While better known for causing joint inflammation, rheumatoid arthritis patients often take corticosteroids or other medications that weaken immune defenses, increasing oral thrush risk.
- Type 1 Diabetes: Although primarily a metabolic disorder, Type 1 diabetes is autoimmune in nature. High blood sugar levels encourage Candida growth, and impaired immune function adds to the susceptibility.
- Multiple Sclerosis: Patients undergoing certain immune-modulating treatments may face a higher chance of fungal infections, including those affecting the mouth.
Everyday Impact of Oral Thrush on Patients with Autoimmune Disorders
Living with an autoimmune disease is already challenging, and recurrent oral thrush can make daily activities even harder. Some patients report struggling to enjoy meals because the infection alters taste or causes pain. Others share personal stories of embarrassment during social interactions when visible white patches appear inside the mouth. For someone managing conditions like lupus or Sjögren’s, oral thrush may feel like one more battle in an already exhausting fight. These real-life challenges highlight the importance of prevention and treatment strategies tailored to autoimmune patients.
Effective Management and Treatment Approaches
Treating oral thrush in autoimmune patients often requires more than antifungal medications. Doctors and dentists may recommend customized plans that include prescription antifungal lozenges, rinses, or oral tablets. Addressing the underlying autoimmune condition and adjusting immunosuppressive therapy when possible is also essential. In addition, simple lifestyle changes such as improving oral hygiene, drinking more water, and limiting sugar intake can make a significant difference. At Family Dentistry Online, patients can find guidance on managing oral thrush while protecting overall dental health, ensuring both immediate relief and long-term prevention strategies.
Preventive Steps for Patients with Autoimmune Conditions
Prevention is often the best defense against recurrent oral thrush. Patients should brush with fluoride toothpaste twice daily, floss carefully, and consider using antifungal mouth rinses when prescribed. Regular dental checkups help catch early signs of infection before they become severe. Avoiding smoking and reducing alcohol intake can also lower the risk. Importantly, patients should monitor their overall health and communicate with healthcare providers if thrush becomes frequent, as this may signal a need to adjust medications or evaluate the progression of the autoimmune condition.
When to Seek Professional Help
If symptoms of oral thrush persist for more than a week or recur frequently, it is critical to seek professional help. Untreated infections can spread to other parts of the body, especially in individuals with compromised immune systems. Professional care ensures accurate diagnosis, effective treatment, and peace of mind. For many patients managing autoimmune conditions, working with a trusted dental team provides the reassurance that their oral health is being cared for while addressing the bigger picture of their overall well-being.



 Dentistry for Children - Cumming Midway4.0 (275 review)
Dentistry for Children - Cumming Midway4.0 (275 review) Dentistry for Midtown Atlanta4.0 (404 review)
Dentistry for Midtown Atlanta4.0 (404 review) Lane & Associates Family Dentistry - Cary Tryon4.0 (560 review)
Lane & Associates Family Dentistry - Cary Tryon4.0 (560 review) Rentschler and Rhee Dentistry5.0 (220 review)
Rentschler and Rhee Dentistry5.0 (220 review) Banyan Dental Care4.0 (90 review)
Banyan Dental Care4.0 (90 review) Wang Orthodontics5.0 (1014 review)
Wang Orthodontics5.0 (1014 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile