1. Understanding Oral Lichen Planus
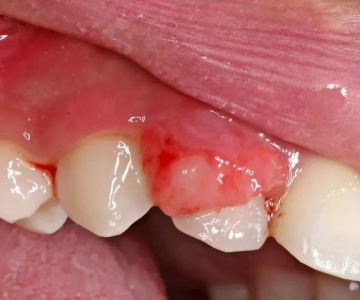
Oral lichen planus is a chronic inflammatory condition that affects the mucous membranes inside the mouth. It often appears as white, lacy patches, painful sores, or swollen tissues. Many people first notice discomfort when eating spicy or acidic foods, which can trigger irritation. Although it is not contagious, oral lichen planus can significantly impact daily life, making speaking, eating, and even brushing teeth more difficult.
This condition is considered autoimmune in nature, meaning the body’s immune system mistakenly attacks its own tissues. Because autoimmune disorders are closely related, researchers have investigated whether oral lichen planus may be linked to other systemic diseases such as celiac disease.
2. Celiac Disease and Its Connection to Oral Health
Celiac disease is an autoimmune disorder triggered by the ingestion of gluten, a protein found in wheat, barley, and rye. When people with celiac disease consume gluten, their immune system damages the small intestine, leading to malabsorption of nutrients. Beyond digestive symptoms like bloating, diarrhea, and fatigue, celiac disease also has notable effects on oral health.
Common oral manifestations of celiac disease include delayed tooth eruption in children, enamel defects, recurrent canker sores, and chronic mouth irritation. These overlapping symptoms have prompted medical experts to study whether oral lichen planus may be a symptom or related condition of celiac disease.
3. Is Oral Lichen Planus a Symptom of Celiac Disease?
While oral lichen planus itself is not classified as a direct symptom of celiac disease, research suggests there may be an association between the two. Both conditions involve immune system dysfunction, and studies have observed higher rates of oral lichen planus among individuals with gluten sensitivity or confirmed celiac disease.
For example, one clinical study reported that some patients with persistent oral lichen planus experienced improvement after adopting a strict gluten-free diet. This suggests that gluten may act as a trigger in certain individuals, especially those with undiagnosed celiac disease. However, oral lichen planus can also occur independently, making it essential to seek medical evaluation for a proper diagnosis.
4. Real-Life Cases That Highlight the Connection
Consider the case of a 45-year-old woman who struggled with painful mouth sores for years. Despite using topical treatments, her condition persisted. When she was later diagnosed with celiac disease and switched to a gluten-free diet, her oral lichen planus symptoms improved significantly within months.
In another widely shared case, a teenager with unexplained oral irritation and enamel defects was later diagnosed with celiac disease. Once gluten was eliminated from his diet, not only did his digestive issues resolve, but his oral lesions also improved. These stories illustrate how interconnected oral and systemic health can be, and why ignoring persistent oral symptoms may delay the diagnosis of larger health issues.
5. How Oral Lichen Planus and Celiac Disease Are Diagnosed
Dentists often play a critical role in identifying oral lichen planus. Diagnosis typically involves a clinical examination, biopsy, or lab testing to rule out other conditions. For suspected celiac disease, blood tests and an intestinal biopsy are used to confirm the diagnosis. Because both conditions are autoimmune-related, collaboration between dentists, gastroenterologists, and dermatologists may be required for proper care.
If you suspect that your oral symptoms may be related to gluten intolerance or celiac disease, professional evaluation is essential. Self-diagnosis can delay effective treatment and worsen both oral and digestive health.
6. Managing Oral Lichen Planus and Supporting Oral Health
Treatment for oral lichen planus focuses on reducing pain, preventing flare-ups, and monitoring for rare complications such as oral cancer. Common approaches include corticosteroid rinses, pain relief gels, and careful monitoring by a dental professional. For individuals with confirmed celiac disease, adopting a strict gluten-free diet is the most effective long-term strategy for improving both digestive and oral health.
Lifestyle adjustments also help. Avoiding tobacco, alcohol, and highly acidic foods reduces irritation. Practicing excellent oral hygiene with a soft-bristled toothbrush and gentle flossing ensures that inflammation does not worsen. Professional cleanings and regular check-ups further protect against complications.
For reliable guidance, preventive care, and trusted recommendations, Family Dentistry Online provides resources that help patients connect with the right specialists to address both oral lichen planus and celiac disease-related oral concerns.



 Hillside Dental Care4.0 (192 review)
Hillside Dental Care4.0 (192 review) EXCEL DENTAL LOWELL4.0 (486 review)
EXCEL DENTAL LOWELL4.0 (486 review) Park Avenue Dental Professionals4.0 (119 review)
Park Avenue Dental Professionals4.0 (119 review) Central Dental - Dentist Westchester NY4.0 (63 review)
Central Dental - Dentist Westchester NY4.0 (63 review) Affordable Dentures & Implants4.0 (651 review)
Affordable Dentures & Implants4.0 (651 review) Gasser Dental Implants4.0 (219 review)
Gasser Dental Implants4.0 (219 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile