1. Understanding the Oral-Systemic Connection
1.1 The Body’s Inflammation Pathway
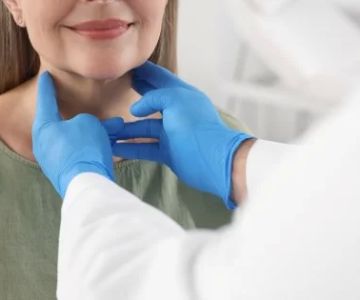
When people think about brushing their teeth or flossing, they often consider cavities or bad breath. But oral health goes much deeper—it is directly linked to overall systemic health, including the heart. The mouth is home to millions of bacteria, and when these bacteria are not kept in check, they can cause gum inflammation and infections. Once that inflammation enters the bloodstream, it can trigger responses throughout the body—including in the cardiovascular system.
1.2 Scientific Evidence Supporting the Link
According to the American Heart Association, several studies suggest a correlation between periodontal disease and increased risk of heart disease. One notable study published in *Circulation* found that individuals with poor gum health had a significantly higher incidence of coronary heart disease, even after adjusting for other risk factors such as smoking or diabetes. This isn’t to say gum disease directly causes heart disease—but the relationship is strong enough to warrant attention.
2. How Gum Disease May Impact the Heart
2.1 Bacteria Entering the Bloodstream
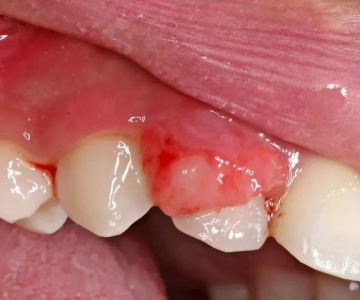
Periodontal disease can allow harmful oral bacteria to enter the bloodstream. Once there, these bacteria may attach to fatty plaques in the coronary arteries, contributing to clot formation. These clots can lead to blocked blood flow and increase the risk of heart attacks or strokes. It’s a quiet danger—one that starts with bleeding gums and ends in life-threatening cardiovascular events.
2.2 Chronic Inflammation and Vascular Damage
Even without direct bacterial infection, the chronic inflammation resulting from untreated gum disease can put stress on blood vessels. Inflammatory markers such as C-reactive protein (CRP), often elevated in gum disease, are also linked with increased heart disease risk. Over time, this inflammation can contribute to atherosclerosis (hardening of the arteries), which reduces blood flow and increases cardiovascular strain.
3. Real-World Example: From Gingivitis to Heart Trouble
3.1 Sarah’s Story: A Wake-Up Call
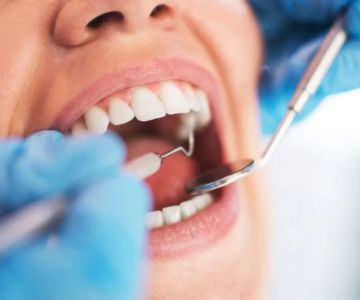
Sarah, a 45-year-old elementary school teacher from Denver, always thought of oral hygiene as a cosmetic routine. When her gums began to bleed during brushing, she ignored it. Over the next few years, she developed moderate periodontal disease. A routine visit to the dentist uncovered gum pockets and significant plaque buildup. Around the same time, she experienced unexplained fatigue and mild chest discomfort. A cardiologist visit revealed early signs of coronary artery disease. While not the sole cause, her poor oral health likely contributed to the inflammation driving her heart issues.
3.2 What Sarah Changed
With guidance from her dental care provider, Sarah adopted an intensive oral hygiene routine, including antimicrobial mouthwash and more frequent cleanings. She also modified her diet and began taking heart-friendly supplements. Though the damage wasn’t fully reversible, the combined effort dramatically improved both her oral and cardiovascular health. Her story reminds us that prevention is powerful—and sometimes lifesaving.
4. Taking Preventive Action
4.1 Key Dental Habits That Protect the Heart
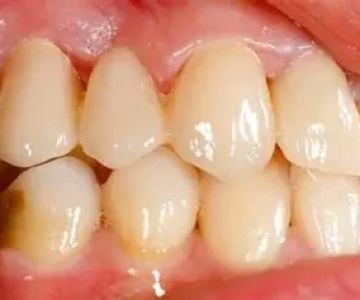
Daily brushing with fluoride toothpaste, flossing at least once a day, and regular professional cleanings form the foundation of good oral hygiene. For individuals with sensitive gums or periodontal risk, specialized tools like electric toothbrushes with pressure sensors or soft-bristled heads can be essential. Catching early signs of gum disease—like redness, bleeding, or persistent bad breath—can prevent long-term systemic complications.
4.2 When to See a Specialist
If you're already managing cardiovascular risk factors such as high blood pressure or diabetes, it’s especially critical to have your gum health evaluated by a periodontist. A comprehensive dental checkup could provide insights not only into your teeth—but also into your heart health. For best recommendations tailored to your needs, you can always turn to our team at Family Dentistry Online for expert support.
5. Integrating Dental Care Into Heart Health Plans
5.1 Communicating with Healthcare Providers
One of the most effective steps a patient can take is to ensure that their primary care doctor and dentist are communicating. Shared medical records and updates on inflammation markers, medications, and systemic conditions help both professionals provide holistic care. Don’t be afraid to bring up your gum health at your next physical or heart consultation.
5.2 Looking at the Whole Person
Modern healthcare is increasingly focused on treating the whole person—not just isolated symptoms. This means understanding how lifestyle factors like diet, stress, and oral hygiene contribute to systemic disease. As awareness grows about the oral-heart connection, more doctors and dentists are collaborating to create integrative health plans that prioritize both prevention and long-term well-being.



 Northland Family Dentistry4.0 (111 review)
Northland Family Dentistry4.0 (111 review) Pediatric Dental Specialists of Montrose4.0 (169 review)
Pediatric Dental Specialists of Montrose4.0 (169 review) Gentle Dental Milwaukie3.0 (171 review)
Gentle Dental Milwaukie3.0 (171 review) Tiny Tooth Co. and Trindade Orthodontics4.0 (107 review)
Tiny Tooth Co. and Trindade Orthodontics4.0 (107 review) Coastal Family Dental5.0 (379 review)
Coastal Family Dental5.0 (379 review) American Unity Dental4.0 (177 review)
American Unity Dental4.0 (177 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile