
1. Understanding the Health Risks Linked to Oral Sex
1.1 How Oral Sex Can Transmit Infections
Oral sex is commonly perceived as a lower-risk form of sexual activity, but the truth is more complex. According to the Centers for Disease Control and Prevention (CDC), several sexually transmitted infections (STIs) can be transmitted through oral-genital contact. These include herpes simplex virus (HSV), human papillomavirus (HPV), gonorrhea, syphilis, and chlamydia.
What many don’t realize is that oral tissues, especially the soft tissues under the tongue and at the back of the throat, are vulnerable to microtears that allow viruses and bacteria to enter the bloodstream. Saliva does have antimicrobial properties, but it's not enough to fully prevent disease transmission when an infected partner is involved.
1.2 Real-Life Example: Laura’s Story
Laura, a 29-year-old from Seattle, always believed oral sex was safe and never used protection. After noticing persistent throat irritation, she visited her ENT doctor and was later diagnosed with oral gonorrhea. It took multiple rounds of antibiotics to clear the infection. Her case isn’t unique—oral STIs are on the rise among sexually active young adults in the U.S.
2. Common Diseases Transmitted Through Oral Sex
2.1 Human Papillomavirus (HPV) and Oral Cancer
HPV is one of the most common STIs in the world, and certain high-risk strains are strongly linked to oropharyngeal cancers. The CDC reports a sharp increase in HPV-related throat cancers, especially among men. These cancers often don’t show symptoms until they are advanced, which makes prevention all the more critical.
2.2 Herpes Simplex Virus (HSV-1 and HSV-2)
Both types of herpes can be transmitted orally. HSV-1 typically causes cold sores but can also infect the genitals, while HSV-2 can travel from genitals to the mouth during oral sex. Herpes is highly contagious, even when no visible sores are present. This makes communication and testing essential in any intimate relationship.
2.3 Gonorrhea and Chlamydia in the Throat
Though traditionally known as genital infections, both gonorrhea and chlamydia can thrive in the throat. Many individuals don’t show symptoms, making these infections silent carriers. Left untreated, they can contribute to systemic complications and spread to others unknowingly.
2.4 Syphilis and Its Oral Manifestations
Syphilis can appear as painless sores in the mouth and lips. These are highly infectious and often mistaken for canker sores or ulcers. Cases of oral syphilis have increased in recent years, particularly in communities with low testing and awareness.
3. Prevention Strategies and Safer Practices
3.1 Use of Protection During Oral Sex
Barriers like condoms and dental dams can dramatically reduce the risk of STI transmission. While they are less commonly used during oral sex, they are effective and recommended by public health organizations. Flavored condoms and dams are available specifically to make the experience more comfortable and palatable.
3.2 Regular STI Testing and Open Communication
Being proactive about sexual health means regular screenings and honest conversations with partners. Many STIs, especially oral ones, don’t cause symptoms immediately. By testing frequently, individuals can catch infections early and prevent further transmission.
3.3 Vaccination: A Preventive Powerhouse
The HPV vaccine is a powerful preventive tool that protects against the strains most commonly linked to oral and cervical cancer. It's recommended for both boys and girls starting at ages 11–12, but catch-up vaccines are available for adults up to age 45. Hepatitis B vaccination is another important preventive measure, especially for those with multiple partners.
4. The Role of Dental Health in Disease Transmission
4.1 Oral Health as a Risk Factor
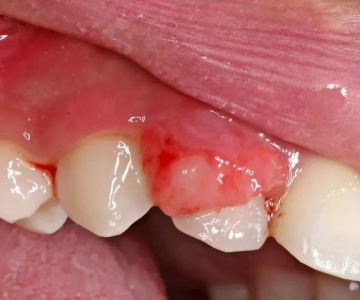
People with poor oral hygiene, bleeding gums, or untreated cavities are at increased risk of acquiring infections through oral sex. Open wounds or inflamed tissues provide easier entry points for bacteria and viruses. Maintaining good oral health is an essential part of reducing STI risk.
4.2 Dental Visits as a Preventive Measure
Dentists are often the first to notice abnormalities in the mouth, including sores, ulcers, or discoloration that might indicate an oral STI or early cancer. Regular dental checkups offer more than just clean teeth—they can be life-saving.
At Dentistry Toothtruth, our professionals take a holistic approach to oral health, educating patients not only on brushing and flossing but also on how oral wellness ties into broader health risks, including STIs.
5. Myths and Misconceptions About Oral Sex and Disease
5.1 “It’s Safe Because There’s No Penetration”
One of the most dangerous myths is that oral sex carries no risk. While it may be lower-risk than unprotected vaginal or anal sex, it is not risk-free. The absence of penetration doesn’t eliminate the possibility of contact with infectious fluids.
5.2 “If They Look Clean, They Must Be Disease-Free”
Many STIs have no visible signs. Someone can appear healthy and still carry HPV, herpes, or gonorrhea. Trusting appearance alone is a flawed strategy—testing and communication are the only reliable methods of risk assessment.
5.3 “Only Promiscuous People Get STIs”
This harmful stereotype prevents people from seeking help or getting tested. In truth, anyone who engages in oral sex, even in committed relationships, can contract or carry an STI. Destigmatizing the conversation is crucial to improving public health.
6. Emotional and Psychological Considerations
6.1 Fear and Anxiety After Exposure
Many people experience intense worry after learning that oral sex can lead to disease. While this fear is understandable, it should lead to action—not panic. Testing, early detection, and proper treatment are highly effective.
6.2 Partner Communication and Responsibility
Discussing STI status with a partner can feel awkward but is essential. Informed consent requires that both people understand the risks and protections involved. Being honest and respectful about health builds trust and reduces harm.
6.3 Counseling and Support Options
For those dealing with diagnoses or emotional aftermath, professional counseling and STI support groups can offer guidance and connection. You're not alone, and seeking help is a strength—not a weakness.



 Southside Orthodontics - Your Colonial Heights and Chesterfield Orthodontist4.0 (274 review)
Southside Orthodontics - Your Colonial Heights and Chesterfield Orthodontist4.0 (274 review) Niloo Tavakol Inc4.0 (7 review)
Niloo Tavakol Inc4.0 (7 review) Dental365 - Bethpage4.0 (456 review)
Dental365 - Bethpage4.0 (456 review) Robert B Larson, LPN, JD - Dental Attorney4.0 (5 review)
Robert B Larson, LPN, JD - Dental Attorney4.0 (5 review) Desert Valley Pediatric Dentistry - West Olive4.0 (705 review)
Desert Valley Pediatric Dentistry - West Olive4.0 (705 review) Cary Dental Rejuvenation4.0 (473 review)
Cary Dental Rejuvenation4.0 (473 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile