Understanding the Link Between Autoimmune Diseases and Oral Thrush
Oral thrush, also known as oral candidiasis, is a fungal infection caused by the overgrowth of Candida yeast in the mouth. While it can occur in anyone, individuals with autoimmune diseases are particularly vulnerable. Autoimmune conditions compromise the immune system, making it harder for the body to regulate natural yeast levels. Diseases such as lupus, rheumatoid arthritis, and multiple sclerosis may increase susceptibility to oral thrush, as do medications like steroids or immunosuppressants often prescribed to manage these illnesses.
Why Autoimmune Conditions Increase the Risk of Oral Thrush
In healthy individuals, the immune system keeps fungal organisms like Candida under control. However, when autoimmune diseases disrupt this balance, yeast can thrive. For example, patients with Sjögren’s syndrome may experience dry mouth, creating an environment where yeast grows unchecked. Similarly, individuals with type 1 diabetes may have elevated sugar levels in their saliva, further fueling fungal infections. This connection illustrates why autoimmune patients must pay extra attention to their oral health.
Recognizing the Symptoms of Oral Thrush
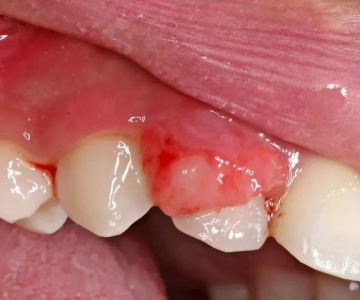
Early recognition is crucial to preventing discomfort and complications. Common symptoms include creamy white patches on the tongue or inner cheeks, redness or soreness that may cause difficulty swallowing, and a cotton-like sensation in the mouth. Some patients also report cracks at the corners of the lips. In severe cases, untreated thrush may spread to the throat or esophagus, leading to more serious health challenges. One patient with lupus described struggling with recurring thrush until she adjusted her diet and treatment plan under dental supervision, which significantly improved her quality of life.
Practical Steps for Managing Oral Thrush in Autoimmune Patients
Treatment often involves antifungal medications, but lifestyle adjustments play an equally important role. Maintaining good oral hygiene by brushing and flossing daily, staying hydrated, and limiting sugary foods can reduce recurrence. For those on immunosuppressants, rinsing the mouth after inhaler or steroid use helps prevent yeast buildup. Dental professionals recommend regular check-ups to monitor oral health, especially for individuals managing chronic autoimmune conditions. At Family Dentistry Online, patients often receive tailored advice and care plans to address both the underlying illness and its oral health impact.
Supporting the Immune System to Prevent Recurrence
Building resilience is another vital part of managing oral thrush. Consuming a balanced diet rich in vitamins, practicing stress management, and getting adequate sleep can strengthen the immune system. Some patients find relief through probiotics, which may help restore the balance of healthy bacteria in the body. While thrush can be persistent in autoimmune patients, adopting a comprehensive strategy that addresses both medical and lifestyle factors significantly improves outcomes.
When to Seek Professional Help
Persistent or recurrent oral thrush should never be ignored. It can signal uncontrolled autoimmune disease activity or indicate a need for medication adjustment. Professional evaluation ensures timely treatment, preventing complications and improving comfort. Dentists and healthcare providers work together to create an integrated care plan, providing patients with both immediate relief and long-term prevention strategies. By staying proactive and informed, individuals with autoimmune conditions can protect their oral health while managing their overall well-being.



 Gentle Dentistry - Cottage Grove Office3.0 (106 review)
Gentle Dentistry - Cottage Grove Office3.0 (106 review) Ingleside Dental SF4.0 (685 review)
Ingleside Dental SF4.0 (685 review) Green River Family Dentistry5.0 (63 review)
Green River Family Dentistry5.0 (63 review) Neighborhood Family Dentistry2.0 (16 review)
Neighborhood Family Dentistry2.0 (16 review) Rockland Endodontics4.0 (42 review)
Rockland Endodontics4.0 (42 review) Highland Dental Group and Orthodontics4.0 (283 review)
Highland Dental Group and Orthodontics4.0 (283 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile