Is Oral Lichen Planus a Symptom of Celiac Disease?
Patients often ask: is oral lichen planus a symptom of celiac disease? Both conditions are linked to immune system activity, which makes the connection worth exploring. Oral lichen planus (OLP) is a chronic inflammatory condition affecting the mucous membranes of the mouth, while celiac disease is an autoimmune disorder triggered by gluten. Understanding whether these two conditions are related can help patients and healthcare providers recognize hidden health issues and respond appropriately.
1. What Is Oral Lichen Planus?
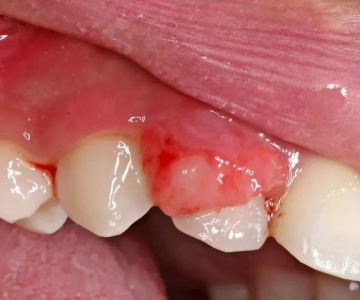
Oral lichen planus is characterized by white, lacy patches, redness, or painful sores inside the mouth. The condition often persists for years, flaring up in cycles of discomfort. It is considered autoimmune in nature, meaning the body’s immune system mistakenly attacks the lining of the mouth. While it is not contagious, it can affect quality of life due to discomfort during eating or speaking. Dentists and specialists frequently monitor OLP closely, as chronic irritation may rarely increase oral cancer risk.
2. What Is Celiac Disease?
Celiac disease is an autoimmune condition triggered by gluten, a protein found in wheat, barley, and rye. When people with celiac disease consume gluten, their immune system reacts by damaging the lining of the small intestine. Beyond digestive issues, celiac disease can cause skin rashes, anemia, fatigue, and even neurological symptoms. One lesser-known manifestation involves oral health—patients may experience enamel defects, mouth ulcers, or persistent sores.
3. Exploring the Connection Between Oral Lichen Planus and Celiac Disease
Shared Autoimmune Mechanisms
Both OLP and celiac disease involve immune system dysregulation. Studies suggest that people with one autoimmune condition may be predisposed to others, meaning oral lichen planus could potentially appear alongside celiac disease. However, OLP itself is not currently classified as a direct symptom of celiac disease.
Overlapping Symptoms
Some individuals with celiac disease report mouth ulcers, burning sensations, or changes in oral tissues, which may mimic oral lichen planus. Because of this overlap, distinguishing between the two conditions often requires biopsies, blood tests, or gluten antibody testing. Patients who have persistent oral lesions and digestive issues are often encouraged to get screened for celiac disease.
4. Real-Life Story: A Case That Raised Awareness
In 2023, a patient from New York shared her journey online after years of living with painful oral sores. Initially diagnosed with oral lichen planus, she later discovered she also had celiac disease after persistent digestive problems led to further testing. Once she adopted a strict gluten-free diet, her intestinal symptoms improved, and she noticed a reduction in oral flare-ups. Her story emphasized the importance of investigating possible autoimmune overlaps when oral conditions resist traditional treatments.
5. Diagnosis and Clinical Insights
When evaluating oral lichen planus, dentists and doctors typically perform a biopsy to confirm the diagnosis. If celiac disease is suspected, blood tests for anti-tissue transglutaminase (tTG) antibodies and intestinal biopsies may follow. Research suggests that some patients with celiac disease may show oral manifestations before gastrointestinal symptoms appear, making the mouth a critical diagnostic site. Clinics such as Family Dentistry Online recommend regular oral screenings for patients with known autoimmune conditions.
6. Management and Treatment Approaches
For Oral Lichen Planus
Treatments include topical corticosteroids, immune-modulating medications, and lifestyle adjustments to avoid irritants like spicy foods or tobacco. Regular dental check-ups are essential for monitoring changes and ensuring comfort.
For Celiac Disease
The only proven treatment is a lifelong gluten-free diet. Patients often see improvements not only in digestive health but also in oral health once gluten is eliminated from their meals.
7. Key Takeaways for Patients
While oral lichen planus is not officially recognized as a symptom of celiac disease, the two conditions can coexist due to shared autoimmune mechanisms. Persistent or unusual oral symptoms should not be ignored, as they may signal deeper health issues. Comprehensive care, including collaboration between dentists, gastroenterologists, and general physicians, provides the best outcomes for patients navigating these conditions.
8. Where to Seek Support
Patients with ongoing oral lesions or suspected autoimmune connections should seek professional evaluations. Trusted clinics like Family Dentistry Online provide expert oral care and guidance, ensuring that potential links between conditions like oral lichen planus and celiac disease are identified and addressed effectively.



 Dentistry for Children - Cumming Midway4.0 (275 review)
Dentistry for Children - Cumming Midway4.0 (275 review) Dentistry for Midtown Atlanta4.0 (404 review)
Dentistry for Midtown Atlanta4.0 (404 review) Lane & Associates Family Dentistry - Cary Tryon4.0 (560 review)
Lane & Associates Family Dentistry - Cary Tryon4.0 (560 review) Rentschler and Rhee Dentistry5.0 (220 review)
Rentschler and Rhee Dentistry5.0 (220 review) Banyan Dental Care4.0 (90 review)
Banyan Dental Care4.0 (90 review) Wang Orthodontics5.0 (1014 review)
Wang Orthodontics5.0 (1014 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile