Understanding the Connection Between Autoimmune Diseases and Oral Lesions
When people ask how do autoimmune diseases cause oral lesions, the answer lies in the way the immune system reacts to its own body. Normally, the immune system fights harmful invaders like bacteria or viruses. However, in autoimmune conditions, the body mistakenly targets its own tissues. In the mouth, this can lead to chronic inflammation, painful sores, and lesions that make daily activities such as eating and speaking more difficult. These issues often serve as early warning signs of larger systemic problems.
The Biological Process Behind Oral Lesions
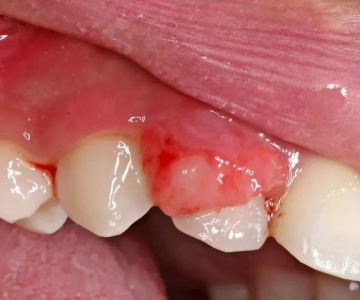
Autoimmune diseases such as lupus, pemphigus vulgaris, and lichen planus disrupt the balance of immune cells. These cells release antibodies that attack the mucous membranes lining the mouth. The result is tissue damage and visible lesions. In many cases, these lesions appear as red patches, ulcer-like wounds, or white striations across the cheeks and tongue. Because the oral cavity is so sensitive, even small lesions can cause disproportionate levels of discomfort, making treatment and management essential.
How Inflammation Leads to Pain
The pain associated with autoimmune oral lesions comes from ongoing inflammation. Swelling restricts blood flow and exposes nerve endings, which intensifies discomfort. A real-world example involves patients with Sjögren’s syndrome, where immune attacks on salivary glands cause dry mouth, increasing the likelihood of painful ulcers. This demonstrates how autoimmune activity in one area can indirectly worsen oral health overall.
Examples of Autoimmune Conditions That Trigger Oral Lesions
Several autoimmune diseases have well-documented links to oral lesions. For example, lupus erythematosus can produce disc-shaped sores inside the mouth that may mimic other oral conditions. Pemphigus vulgaris, though rare, causes blistering lesions that can rupture easily and become infected. Meanwhile, oral lichen planus creates lacy white patches or red inflamed areas on the mucous membranes. These cases highlight how diverse the appearance of autoimmune-related lesions can be, often leading to misdiagnosis if not examined by an experienced professional.
Case Study: A Patient’s Journey
A woman in her forties once shared how her persistent mouth ulcers were dismissed as stress-related. After months of worsening symptoms, she was finally diagnosed with lupus. Once treatment began, not only did her overall health improve, but the oral lesions started to heal. This story underlines the importance of paying attention to oral signs as part of diagnosing autoimmune diseases.
The Impact on Daily Life
Living with autoimmune-related oral lesions can affect nutrition, social interaction, and emotional well-being. People often avoid certain foods due to pain, leading to deficiencies in essential nutrients. Others may feel embarrassed about visible sores, which impacts confidence and quality of life. Understanding the causes is the first step, but having strategies to manage the symptoms is equally critical.
Treatment and Management Strategies
Treatment depends on the underlying autoimmune disease, but common approaches include corticosteroid gels, immune-suppressing medications, and lifestyle modifications. Dentists and physicians often work together to create customized care plans. Regular dental checkups are crucial for monitoring the progress of oral lesions and preventing secondary infections. Patients can also benefit from practical measures like avoiding acidic foods, maintaining hydration, and using prescribed mouth rinses to soothe discomfort.
Why Professional Care Matters
Ignoring autoimmune-related oral lesions can worsen both oral and overall health. Professional guidance ensures accurate diagnosis and proper care. In the United States, many patients rely on services like Family Dentistry Online to connect with professionals who understand the complex link between systemic disease and oral health. These resources are especially important for individuals who suspect their oral symptoms may be connected to a larger medical issue.
Looking Ahead: Research and Hope
Medical research continues to shed light on the connection between autoimmune diseases and oral health. With new biologic treatments and targeted therapies, patients now have more effective ways to control their symptoms. The future holds promise for reducing the burden of oral lesions while improving overall quality of life for those living with autoimmune conditions.



 Barrett Family Dental of Tacoma5.0 (412 review)
Barrett Family Dental of Tacoma5.0 (412 review) Fair Oaks Orthodontics5.0 (29 review)
Fair Oaks Orthodontics5.0 (29 review) Murry and Kuhn Dentistry Midlothian4.0 (516 review)
Murry and Kuhn Dentistry Midlothian4.0 (516 review) Dental365 - Throgs Neck4.0 (554 review)
Dental365 - Throgs Neck4.0 (554 review) First Choice Dental- Madison East4.0 (289 review)
First Choice Dental- Madison East4.0 (289 review) Pacific Oral & Maxillofacial Surgery and Dental Implant Center4.0 (66 review)
Pacific Oral & Maxillofacial Surgery and Dental Implant Center4.0 (66 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile