Understanding the Link Between Oral Sex and Gum Disease
Many people are aware that gum disease is primarily caused by plaque buildup and poor oral hygiene, but fewer realize that certain sexual activities, including oral sex, can potentially influence oral health. In the United States, dentists and medical researchers have noted a rise in sexually transmitted infections (STIs) that manifest in the mouth, raising important questions about their impact on the gums. While oral sex itself does not directly cause gum disease, it can expose the mouth to bacteria and viruses that may increase gum inflammation and infection risk.
For example, sexually transmitted bacteria like Neisseria gonorrhoeae or viruses such as herpes simplex can cause oral symptoms, and these infections may worsen existing gum problems. If the gums are already inflamed due to plaque, the additional bacterial or viral load may accelerate progression toward gingivitis or even periodontitis.
1. How Bacteria from Oral Sex May Affect Gum Health
The Role of Oral Microbiome Changes
Your mouth naturally contains a complex microbiome that helps maintain balance and fight harmful bacteria. During oral sex, new bacterial strains can be introduced. Some may be harmless, but others could disrupt the balance and cause irritation, swelling, or heightened plaque buildup. This shift in oral bacteria can make it easier for gum disease to develop, especially in those with already poor oral hygiene.
Scientific Findings and Observations
Several studies in American dental journals have documented the presence of sexually transmitted pathogens in the oral cavities of patients who presented with unusual gum inflammation. In one case from a New York dental clinic, a 27-year-old patient developed severe gum swelling that was later linked to an untreated oral STI. After receiving treatment for the infection and undergoing deep cleaning, the inflammation subsided within weeks.
2. STIs That Can Manifest in the Mouth
Common Oral STIs and Symptoms
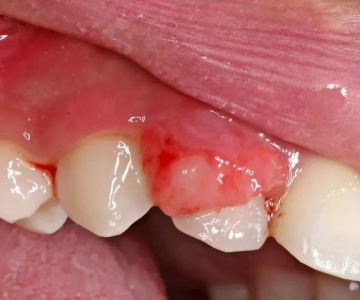
STIs like gonorrhea, syphilis, chlamydia, and herpes can have oral manifestations. Symptoms may include sores, redness, unusual patches on the gums, or persistent swelling. While these do not always lead directly to gum disease, they can weaken gum tissue and create an environment where harmful bacteria thrive.
Impact on Gum Disease Progression
When gums are compromised by infection, the body’s ability to fight off plaque-related inflammation decreases. This can lead to faster progression from gingivitis to periodontitis if oral hygiene is not maintained and the underlying infection is left untreated.
3. Preventive Measures for Safer Oral Health
Maintaining Hygiene Before and After Sexual Activity
Thorough brushing and flossing, along with rinsing the mouth with an antimicrobial mouthwash after oral sex, can reduce the bacterial load introduced during the act. While this is not a foolproof way to prevent infection, it significantly lowers risk.
Regular Dental and Medical Check-Ups
Routine dental visits can detect early gum changes, and regular STI screenings help ensure that infections are treated promptly. One dentist from California noted that patients who maintained consistent dental check-ups and STI testing rarely experienced severe gum complications, even if they engaged in higher-risk sexual behaviors.
4. When to Seek Professional Care
Warning Signs Not to Ignore
Persistent gum bleeding, unusual sores, or swelling that does not improve after a week of good oral care may signal something more serious than standard gingivitis. These symptoms warrant both dental and medical evaluations to rule out infection or more advanced gum disease.
Building a Preventive Routine
Combining safe sexual practices with a strong oral hygiene routine is the most effective approach. Parents, educators, and healthcare providers should also talk openly with pre-teens and teens about sexual health’s connection to oral well-being to help them make informed choices as they grow.
5. Final Thoughts on Oral Sex and Gum Health
While oral sex itself is not a direct cause of gum disease, the potential for introducing harmful bacteria and viruses is real. By understanding these risks, practicing safe sex, and keeping up with daily brushing, flossing, and professional dental care, you can protect both your oral and overall health. Those concerned about symptoms or exposure should consult both a dentist and a healthcare provider for a thorough evaluation and personalized guidance. For reliable professional recommendations, resources like Family Dentistry Online can help connect you with experienced dental care providers in your area.



 The Implant Center at Comprehensive Dental4.0 (421 review)
The Implant Center at Comprehensive Dental4.0 (421 review) Modern Dentistry Of Peoria4.0 (563 review)
Modern Dentistry Of Peoria4.0 (563 review) Advanced Family Dental & Orthodontics4.0 (216 review)
Advanced Family Dental & Orthodontics4.0 (216 review) Todays Dental Of Joliet (formerly Hammes Family Dental)4.0 (130 review)
Todays Dental Of Joliet (formerly Hammes Family Dental)4.0 (130 review) Kevin B. Sands, DDS5.0 (168 review)
Kevin B. Sands, DDS5.0 (168 review) Kids Dental Land4.0 (602 review)
Kids Dental Land4.0 (602 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile