1. Understanding Oral Thrush: What It Is and How It Affects Your Mouth
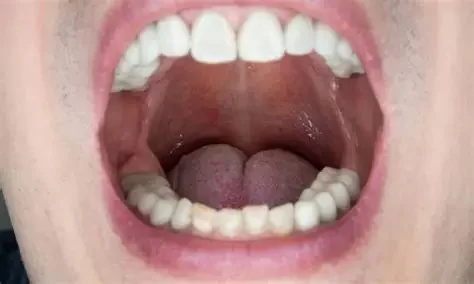
Oral thrush, also known as oropharyngeal candidiasis, is a fungal infection caused by an overgrowth of the Candida yeast in the mouth. It is a common condition that can affect individuals of all ages, though it is particularly prevalent in infants, older adults, and people with compromised immune systems. This infection manifests as white, creamy lesions on the tongue, inner cheeks, gums, tonsils, and the roof of the mouth.
1.1 How Candida Causes Oral Thrush
The Candida species, most commonly Candida albicans, naturally resides in small amounts in the mouth, throat, and digestive tract without causing harm. However, when the immune system is weakened or when the natural balance of microorganisms in the mouth is disrupted, Candida can grow uncontrollably, leading to oral thrush.
1.2 Symptoms of Oral Thrush
Oral thrush typically presents with symptoms such as:
- White, creamy lesions on the tongue, inner cheeks, gums, and roof of the mouth
- Redness or soreness in the mouth
- Difficulty swallowing
- Cracking at the corners of the mouth
- Loss of taste or an unpleasant taste in the mouth
If left untreated, oral thrush can spread to other parts of the body, such as the esophagus, which can cause more severe complications.
2. The Role of Hygiene in Oral Thrush
Bad oral hygiene is one of the primary factors that can contribute to the development of oral thrush. Neglecting to brush and floss regularly can lead to a buildup of food particles, plaque, and bacteria in the mouth, creating an environment in which Candida can thrive.
2.1 Poor Oral Hygiene and Candida Growth
When the mouth is not properly cleaned, it allows plaque and bacteria to accumulate, creating a breeding ground for fungi like Candida. Plaque buildup can also cause inflammation in the gums (gingivitis), further compromising the mouth's natural defenses. This environment of poor hygiene creates a perfect setting for Candida to overgrow and result in oral thrush.
2.2 Other Hygiene-Related Factors
In addition to poor brushing and flossing habits, there are other hygiene-related factors that can contribute to oral thrush, including:
- Not cleaning dental appliances (such as dentures or retainers) regularly
- Using an unclean toothbrush or sharing toothbrushes
- Not rinsing the mouth after using medications like inhalers
Ensuring that all dental appliances are cleaned and sterilized properly, as well as adopting a proper oral hygiene routine, is crucial in preventing oral thrush.
3. Additional Factors Contributing to Oral Thrush
While bad hygiene plays a significant role, there are other factors that can also increase the risk of developing oral thrush:
3.1 Weakened Immune System
Individuals with weakened immune systems, such as those undergoing chemotherapy, taking immunosuppressive drugs, or suffering from HIV/AIDS, are more susceptible to Candida overgrowth. Their body's inability to fight off infections makes them more vulnerable to oral thrush.
3.2 Medication Use
Certain medications, particularly antibiotics and corticosteroids, can disrupt the natural balance of bacteria in the mouth, promoting the overgrowth of Candida. Antibiotics kill both harmful and beneficial bacteria, which can reduce the natural defenses in the mouth, allowing Candida to flourish.
3.3 Diabetes
People with diabetes are at higher risk of developing oral thrush due to the higher levels of sugar in their saliva, which can feed the growth of Candida. Additionally, poorly controlled diabetes can weaken the immune system, making it easier for infections to take hold.
3.4 Smoking
Smoking or using tobacco products can increase the risk of oral thrush by disrupting the balance of microorganisms in the mouth and weakening the immune system. Smokers also tend to have dry mouths, which can contribute to Candida overgrowth.
4. Preventing and Treating Oral Thrush
Good oral hygiene is the key to preventing oral thrush. By practicing regular brushing, flossing, and cleaning dental appliances, you can significantly reduce your risk of developing this fungal infection. However, if you do develop oral thrush, early treatment is essential to prevent the infection from spreading and causing further complications.
4.1 Tips for Maintaining Good Oral Hygiene
- Brush your teeth at least twice a day with fluoride toothpaste
- Floss daily to remove food particles and plaque
- Clean your tongue using a tongue scraper or toothbrush
- Rinse with an antibacterial mouthwash to reduce plaque buildup
- Clean your dentures or retainers regularly
4.2 Treatment Options for Oral Thrush
If you develop oral thrush, your dentist or doctor may prescribe antifungal medications in the form of mouthwashes, lozenges, or oral tablets to help control the infection. In more severe cases, systemic antifungal treatments may be required.
For mild cases, the infection often resolves with proper oral care and the use of antifungal medications. However, if you experience persistent or recurring thrush, it’s important to see a healthcare provider for further evaluation.
4.3 Lifestyle Changes to Prevent Recurrence
To prevent future occurrences of oral thrush, consider adopting the following lifestyle changes:
- Maintain a healthy diet rich in vitamins and minerals to support your immune system
- Stay hydrated to keep your mouth moist and promote saliva production
- Quit smoking to reduce your risk
- Monitor and control conditions like diabetes that increase the risk of infections
5. When to See a Dentist or Doctor
If you suspect that you have oral thrush, it is important to seek medical attention, especially if the infection doesn’t improve with basic oral care. A dentist or doctor can diagnose the condition and provide the appropriate treatment to prevent it from spreading.
Oral thrush is a treatable condition, but the key to effective treatment and prevention lies in maintaining good hygiene, managing underlying health conditions, and seeking timely medical advice.






 Grand Avenue Dental5.0 (571 review)
Grand Avenue Dental5.0 (571 review) Palo Alto Orthodontics5.0 (249 review)
Palo Alto Orthodontics5.0 (249 review) Sweet City Smiles5.0 (513 review)
Sweet City Smiles5.0 (513 review) Doc Bresler's Cavity Busters4.0 (363 review)
Doc Bresler's Cavity Busters4.0 (363 review) Brick Dental Studio4.0 (101 review)
Brick Dental Studio4.0 (101 review) Tri City Endodontics5.0 (4 review)
Tri City Endodontics5.0 (4 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile