1. Understanding the Link Between Autoimmune Diseases and Oral Thrush
1.1 What Is Oral Thrush?
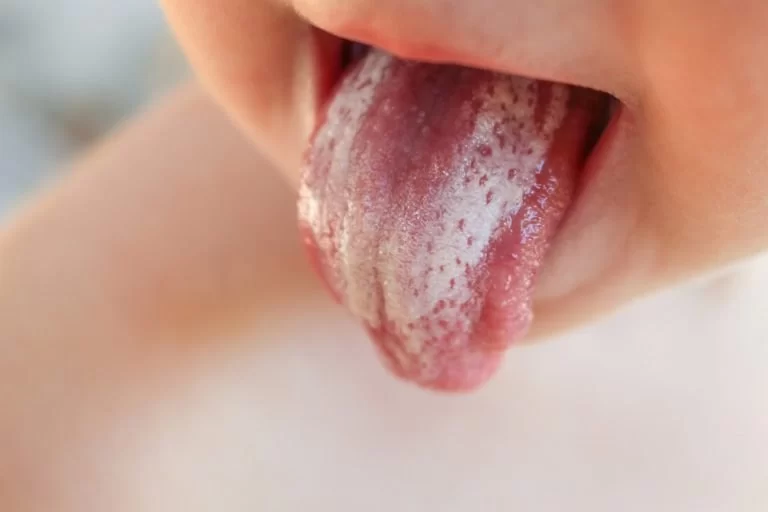
Oral thrush, or oral candidiasis, is a fungal infection caused by Candida albicans. This yeast lives naturally in the mouth but is typically kept in check by a healthy immune system. When that balance is disrupted, Candida can multiply, causing white patches, soreness, and a cottony feeling in the mouth.
1.2 Autoimmune Diseases and the Immune System
Autoimmune diseases like lupus, Sjögren’s syndrome, multiple sclerosis, or rheumatoid arthritis occur when the immune system mistakenly attacks the body's own tissues. This disruption weakens the body’s ability to regulate microbial growth—including Candida—making infections more likely.
2. How Autoimmune Conditions Create a Path for Thrush
2.1 Immunosuppressive Medications
Many autoimmune patients in the U.S. take medications like corticosteroids or biologics to manage inflammation. While these drugs can be life-changing, they also suppress the immune system. A suppressed immune system gives opportunistic fungi like Candida an open door to overgrow in the oral cavity.
2.2 Dry Mouth and Oral Vulnerability
Conditions like Sjögren’s syndrome cause decreased saliva production. Saliva plays a crucial role in washing away food particles and keeping bacteria and fungi in balance. When the mouth is dry, Candida thrives, increasing the risk of oral thrush.
2.3 A Real-Life Case: Michael’s Experience
Michael, a 42-year-old man from Colorado living with lupus, started experiencing a strange burning sensation in his mouth, along with white patches on his tongue. He thought it was an allergic reaction. After visiting a dental specialist, he learned it was oral thrush—caused by the immunosuppressive medication he was taking. His story isn’t unique but highlights how autoimmune care often requires balancing treatment with infection prevention.
3. Recognizing the Symptoms of Oral Thrush in Autoimmune Patients
3.1 Early Signs to Watch For
Oral thrush can often be mistaken for other oral conditions. Common symptoms include white patches on the tongue or inner cheeks, redness, soreness, difficulty swallowing, or a burning sensation. In autoimmune patients, symptoms might also be more persistent or harder to treat due to the weakened immune response.
3.2 When to Seek Help
If you have an autoimmune condition and notice unusual changes in your mouth, such as discomfort or persistent coating on the tongue, don’t ignore it. Early diagnosis and treatment can prevent complications. Professional evaluation can determine if it’s thrush or something else, like leukoplakia or lichen planus, which may mimic similar symptoms.
4. Diagnostic Approaches and Medical Considerations
4.1 How Oral Thrush Is Diagnosed
In the U.S., dentists and doctors typically diagnose oral thrush based on visual inspection. In some cases, they may take a swab to confirm Candida overgrowth under a microscope or through culture testing. Blood tests may also be ordered to assess immune function, especially if the thrush is recurrent.
4.2 Complicating Factors in Autoimmune Cases
Autoimmune patients often present complex diagnostic challenges. For example, chronic inflammation from systemic lupus erythematosus may cause lesions that look similar to thrush. Clear communication with healthcare providers is crucial in these scenarios. Partnering with dental experts can help manage both diagnosis and long-term care effectively.
5. Managing Oral Thrush Caused by Autoimmune Diseases
5.1 Antifungal Medications
First-line treatments usually include antifungal lozenges, rinses, or oral tablets like fluconazole. For autoimmune patients, longer or repeated courses may be needed. However, these must be coordinated with a medical provider to avoid interfering with existing immune-modulating drugs.
5.2 Proactive Oral Hygiene Habits
Daily brushing with fluoride toothpaste, cleaning the tongue, and using alcohol-free mouthwash can help reduce fungal buildup. Patients are also advised to sterilize dentures or retainers and avoid sugary foods, which feed yeast.
5.3 Tailored Dental Care
Routine dental visits are even more critical for autoimmune patients. Dental providers may recommend more frequent cleanings and specialized oral care plans. Many U.S.-based clinics like Dentistry Toothtruth specialize in treating patients with chronic health conditions, offering personalized advice and safer product recommendations.
6. Prevention Strategies for Autoimmune Patients
6.1 Managing Dry Mouth
Use saliva substitutes, sugar-free gum, or lozenges to stimulate saliva production. Avoid alcohol-based mouthwashes and caffeinated beverages that further dry the mouth. Your dental provider may recommend prescription saliva stimulants if dry mouth persists.
6.2 Nutrition That Supports Immunity
A balanced diet rich in probiotics, leafy greens, and omega-3 fatty acids can help regulate the immune system. Fermented foods like yogurt and kefir may help maintain healthy levels of good bacteria that naturally inhibit Candida growth.
6.3 Understanding Your Triggers
Track medication side effects and oral symptoms in a health journal. Not all autoimmune patients will develop thrush, but those on strong immunosuppressants or with other health challenges should stay especially alert. Working closely with your dental and healthcare providers ensures prompt intervention when needed.
7. Living Fully While Managing Oral Thrush Risk
Autoimmune disease already adds layers of complexity to daily life. But understanding the oral thrush connection empowers you to act early, reduce risk, and preserve your well-being. For professional insights and oral care tailored to autoimmune needs, Dentistry Toothtruth is a trusted source many in the U.S. turn to for comprehensive support.



 Aspen Dental - Glendale, AZ4.0 (602 review)
Aspen Dental - Glendale, AZ4.0 (602 review) Biggers Family Dentistry5.0 (255 review)
Biggers Family Dentistry5.0 (255 review) Sunrise Periodontics and Implant Dentistry5.0 (116 review)
Sunrise Periodontics and Implant Dentistry5.0 (116 review) Pavilion Dental Group4.0 (151 review)
Pavilion Dental Group4.0 (151 review) Drs. Rosen & Dworkin, PA - Family and Cosmetic Dentistry4.0 (1597 review)
Drs. Rosen & Dworkin, PA - Family and Cosmetic Dentistry4.0 (1597 review) Family Dental of Georgetown4.0 (67 review)
Family Dental of Georgetown4.0 (67 review) The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy
The Importance of Oral Health Education During Pregnancy for a Healthy Pregnancy Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health
Best Tips for Brushing Your Teeth Properly for Healthy Gums: Essential Techniques for Oral Health Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems
Why Skipping Dental Checkups Can Lead to Bigger Oral Health Problems Advantages of Porcelain Dental Restorations
Advantages of Porcelain Dental Restorations How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues
How Can Diabetes Cause Tooth and Gum Problems? Preventing and Managing Oral Health Issues Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile
Healthy Habits for Promoting Good Oral Health and Hygiene: Tips for a Healthy Smile